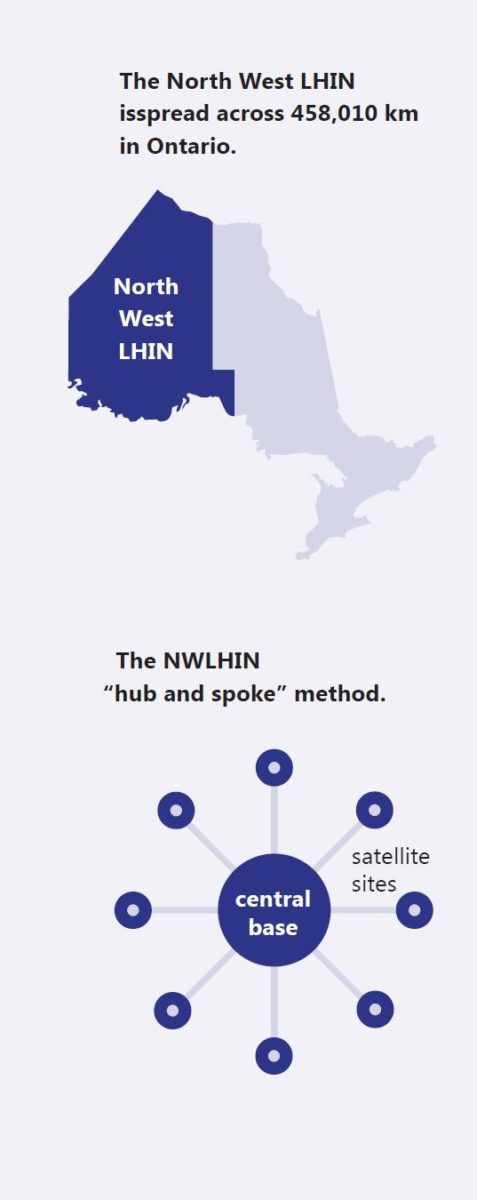
Imagine a geographical area the size of France being served by one over-worked Health Sciences Centre and three community hospitals.
That’s the challenge that faces Northwestern Ontario every day.
While the population is far less than that of France, many unique factors impact healthcare delivery.

Harsh Driving Conditions and Vast Distances
Winters in Northern Ontario are no picnic. If a patient has to drive from Dryden to Thunder Bay for a consultation visit, the journey will cover over 340 kilometres and take nearly four hours on clear roads — one way. Winter weather is notorious for heavy snow and bitter wind chills, so a round trip of 8 hours is an arduous but common task.
The Northwest region includes the centres of Dryden, Kenora, Fort Frances and Thunder Bay and all small towns and villages in between. Three years ago, the Northwest region took a different approach to try to serve the vast distances in their region more effectively while attempting to reduce surgical wait times¹.
They devised what Caroline Fanti, Program Director for the Regional Orthopaedic Program calls a “hub and spoke” method. “We have one centralised team based in Thunder Bay that provides care to the three other satellite sites on a monthly basis” for hip and knee replacement surgeries. “We’d do consults, new assessments, and follow up care and do that work at the satellite sites,” she explains.
An Outmoded Referral System
The challenge was made more difficult by the traditional method of patient referral in the Ontario healthcare system: a primary care provider with a patient needing surgery, for example, would fax a service request to an individual surgeon’s office. Often, the primary care physician would send out several faxes to different surgeons, hoping that one of them would be able to book a consult as soon as possible without having any idea – or any feedback – that it would happen.
Worse, Fanti says, was how often referrals for hip or knee replacements would end up on the desk of a surgeon specialising in shoulder procedures where they would sit for a couple of months before getting sorted out. Despite outreach, the region saw its wait times remaining high because of the inefficiencies inherent in the referral system. Even the establishment of a Regional Joint Assessment Clinic (RJAC) in 2011 didn’t solve the issue because doctors continued to send referrals directly to surgeons, the RJAC itself or to specialty clinics in Fort Frances and Kenora, hoping that someone would act on the request.
“Plus, there were no time mandates or coordination on these requests,” Fanti points out. “There were many occasions when we’d see a patient in Thunder Bay who had travelled to see us and we’d be going to their community the following week and the patient had no idea! They’d drive maybe 6 hours to get here on bad highways.”
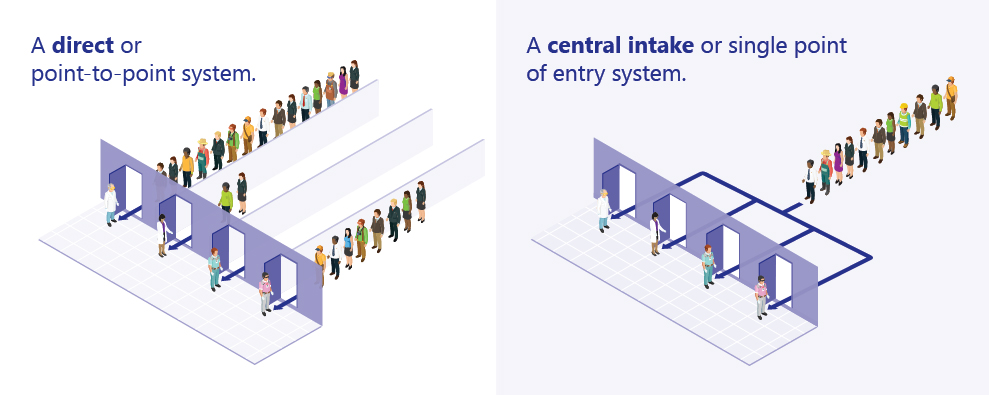
Making Inroads with Novari Health and Central Intake
That all began to change on April 1, 2018. That was the date when the NWLHIN implemented Novari Health’s award-winning software technology called Novari eRequest. The cloud-based technology allows for a highly efficient and accountable Central Intake (CI) system.
Today, every referral MUST come through the CI system to the assessment centre or it won’t be actioned. When a service request arrives, an advanced practice physiotherapist triages the referral, based on the patient’s accompanying records and where the patient lives.
“So, we can determine who’s a higher priority, if we’re going to see the patient here in Thunder Bay or via telemedicine, or if we can see them in a few weeks when our team is in their area. We can do all this centrally for all the communities we serve,” Fanti states. “We’ve changed the name from Joint Assessment Clinic to Rapid Action Centre because our mandate is to see patients quickly. We’re trying to minimise patient travel time as much as possible, as well.” There is no question in her mind how the Novari eRequest and Access to Care technologies have impacted the Northwest.
“Novari can tell me at the end of the day ho wmany hip replacements were done that daya nd how many have been done in whatever time frame I want. This is far more accurate and rapid data than we’ve ever had before.”
— Dr. David Puskas, Ortho Surgeon, Thunder Bay Regional Health Sciences Centre
Dramatic Drop in Wait Times with Novari
“Novari in concert with our Central Intake has brought down Wait 1 times for consult to under four weeks,” she states. “We’re now among the best performing [regions] when it comes to Wait 1. Our Wait 1B times for surgery are number one in the province, according to Cancer Care Ontario.”
This view is echoed by Dr. David Puskas, a top orthopaedic surgeon at Thundery Bay Regional Health Services Centre. “The Novari solution allowed us to take our program and actually turn it into a business model which has given us enormous credibility with both our hospital, our [region] and the Ministry of Health. As a direct result, we have more money being fed into our program than we would have had otherwise.”
The Business Case for Novari
The idea that Novari’s technology does more than streamline efficiencies but actually saves money and wasted effort, is a strong business argument. As Dr. Puskas puts it, “this is the era of business plans and evidence-based queries to the Ministry. The Novari ATC and eRequest modules allows us to actually understand what’s waiting where and how to match the human
resources to manage the inflow into the system as well as the outflow in the operating rooms. I can tell on a day to day basis how many hips and knees have been done and I can project how many cases a week I can manage if my Wait 1 times are within the acceptable range and
how many cases a week I have to generate to get my Wait 2 times under control. We’ve never been able to meet either of these before. This is entirely due to the Novari ATC solution because there’s nowhere else I’m going to get that data.”
Optimised Operating Room's Now a Reality
One of the many key strengths of the Novari platform, according to Dr. Puskas, is how well it organises and predicts operating room schedules. Very often in the hospital, he explains, surgeons would argue that they needed more OR time because they had so many cases that were backing up.
“Then, all of a sudden, ATC comes along and tells us what the actual number of cases waiting is as well as the time to clearance for those cases. This is great to know because now we’re dealing with real data. So, when we present our business plans to the hospital, we can show them that we saved enough money in efficiencies to fund a hundred more primary joint replacements, for example.”
Caroline Fanti likes to point to how well Novari helps prevent lost OR time, as well. “We had a patient in Thunder Bay who’d been waiting for a long time and our facility in Dryden got on the Novari platform, discovered the patient waiting in Thunder Bay and offered them an open OR slot in Dryden. If you’re wasting OR times, you’re also driving up wait times. We can see every patient in the Northwest on Novari and know how long every patient has been waiting, thanks to their ATC system.”
Governments know how easily money can be wasted. The temptation in a healthcare system like Ontario’s is to throw more money at what is perceived to be the problem: lack of surgeons, too few ORs, not enough beds. Novari Health’s Access to Care technology has demonstrated in Thunder Bay, Dryden, Kenora and Fort Frances exactly what it’s been demonstrating in hospitals and health authorities across Ontario for a number of years: leverage technology to drive efficiency and, not only does the healthcare system run far more smoothly with dramatically reduced wait times but money can be saved, rather than spent.
1 https://www.cbc.ca/news/canada/kitchener-waterloo/compare-ontario-hospitalwait-
times-online-regional-variance-1.4249141

